

About
Advanced Therapy & Wellness Center is a holistically-based and wellness-oriented clinic with focus on delivery of premium therapy services to children and adults whose lives have been impacted by speech, language, cognitive, feeding/swallowing, orofacial myofunctional, and/or breathing pattern disorders as well as physical limitation and chronic disease.
Services
In our approach, we acknowledge that everyone has their own individual story and come from different walks of life. For this reason, we take down in-depth background information to learn about what you have already been through in the past. Whether you've been consulted by a doctor or just heard something from a mom's group, we want to hear your concerns and instincts about your health or the health of your child. We take that information and pair it with our professional examination to get at the root of your concerns. Once we identify what is causing your struggles, we plan an individual path to help you reach YOUR best potential for the future.


PEDIATRIC THERAPY
We work closely with you, your child’s teachers, other therapists, and doctors to provide treatment that fits your child's specific needs. We help your child build a brighter future through confidence and improved function.
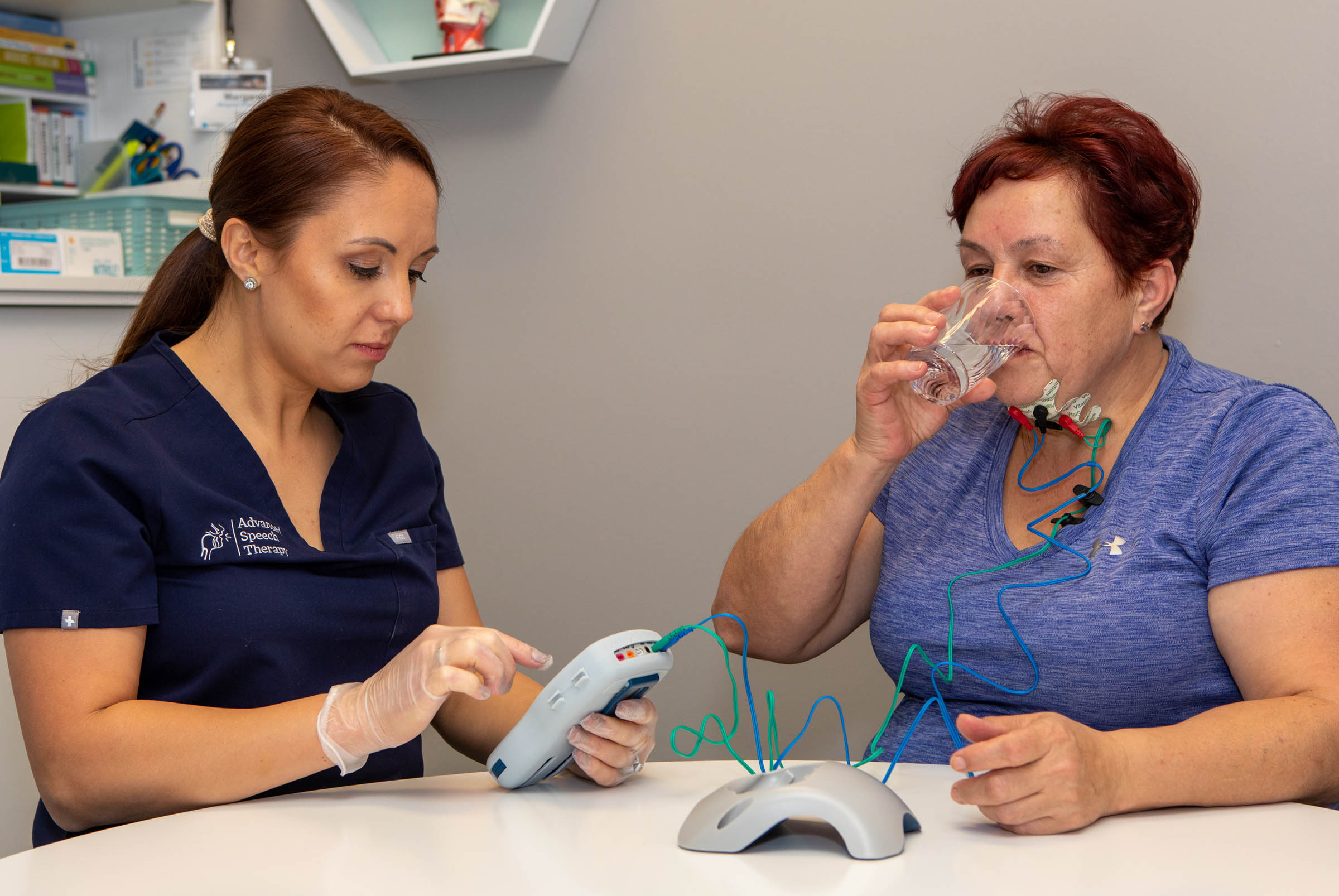
ADULT THERAPY
We help adults regain speech, language, and/or cognitive skills as well as swallowing functionality following stroke, TBI, or cancer. We also work with adults suffering from progressive diseases such as Parkinson's disease, MS, and ALS.

MYO
Strong signs that indicate a myofunctional disorder in a child can include open mouth posture, mouth breathing, crowded teeth, narrow palate, small jaws, a protruding tongue, visible at rest, during eating and during speech.
HOLISTIC HEALTH
Have you ever wondered why human beings are aging so fast on a physical level? Simply, people have been programmed to eat unhealthy food. There has never been a time in history where people have consumed so many drugs and received so many surgeries and implants.
WOLFE NON-SURGICAL
All problems within the body stem from an inflammation and scar tissue issue, right from the tip of your nose to the end of your toes.
NUTRITIONAL & EMOTIONAL CONSULTATION
The Perfect Day consultations offer nutritional and emotional coaching that will allow you to create a perfect day, every day. Benefits include:

ENERGY MEDICINE
Energy medicine is a field of complementary therapy based on the interactions of the human energy field with other energy fields (human or other). The human body is surrounded by and emits various kinds of energy: electrical, magnetic, light, and subtle.
CELLSONIC
The CellSonic VIPP machine is a new branch of medicine that kills infection and triggers tissue regeneration.
AVECEN
It is FDA- Cleared Class ll medical device that uses technology developed by AVACEN Medical.
BIOPTRON
BIOPTRON light improves cell metabolism and initiates biological and cellular reactions in a process known as photo-biostimulation.
VIT D LIGHT
Crystal Light Therapy is the SolRx E-Series UVB-Narrowband full body system with quartz crystal panels.
TESTIMONIALS
My son’s speech therapist is doing a great job. She is very patient and has completely gained his trust and attention. My son loves going to his speech therapy and likes doing the speech exercises even at home!
- Biljana P 2/15/22
My daughter started going to Advanced Therapy & Wellness Center about 4 months ago when we suspected she had oral ties. Margaret is amazing, she is clearly an expert in her field and has so much experience treating infants. When my daughter is struggling with feeding, she always has great suggestions on things to try. And they always work! She has made a real impact in my daughter's life and I'm so thankful for the work she does.
- Kristah K 2/1/22
Margaret, thank you for today's session. Such a unique feeling, painful as well and I really don't know what happened but it just felt good. I was crying also the whole way back home.
- Beata, Wolfe Non-Surgical Patient
Advanced Therapy & Wellness literally saved our nursing journey! Our baby was taking so long to eat that he’d tire himself out, fall asleep and be hungry again in an hour. He was so fussy and I knew it was more than typical baby fussiness. I researched feeding therapists near me and was so lucky to find Advanced Therapy & Wellness Center. I was so impressed with her knowledge, her amazing demeanor and care for our son, and her ability to detect exactly what was going on. She noticed our sons lip and tongue ties and referred us to a pediatric dentist for revision. She provided pre an post treatment and gave us home exercises for carryover. Our baby went from taking forever to feed and never getting full to transferring 4 ounces with ease! We will forever be grateful for Advanced Therapy & Wellness Center!
- Shaina N 2/14/22
My son’s myofascial therapist is fantastic. She is gentle and fun but also makes sure he is progressing and working hard during his therapy sessions and at home. She always makes sure we both fully understand everything that is going on. We drive 45 minutes each way weekly for their office and will continue to do so as long as we need to. I love their holistic approach. The front desk staff is friendly and helpful. I highly recommend this office.
- Aubrey R 9/18/21
I highly recommend Ms Margaret for speech therapy. After seeing many therapists she was the first to actually identify some of the issues and truly support and guide us through a tongue tie revision. She has been working with my son for over six months and I couldn't be happier. She's patient, professional and caring. I feel so blessed to have her working with my son and would highly recommend her to anyone!!!
- Malgorzata S














